Vasculitis is an inflammation of blood vessels in the body. It happens when the blood vessels are incorrectly targeted by the immune system, whether due to an infection, medication, or another disease. This can restrict blood flow and cause damage to tissues and organs.
This can damage veins, arteries, and capillaries. When a blood vessel gets inflamed it can:
- Make it difficult for blood to flow through, as the vessel gets smaller
- Close completely, to avoid blood from flowing through
- Stretch and so much weak that it bulges. It is known as an aneurysm and can cause severe bleeding inside the body if it bursts.
Several forms of vasculitis exist but most are rare. Vasculitis, however, may affect one or more organs, and maybe long-lived (chronic) or short-lived (acute). Although certain forms of vasculitis are more common in certain groups of people and among those suffering from specific diseases, this disorder can affect everyone.
Symptoms
Symptoms of vasculitis may result from direct damage to the blood vessels or indirect damage to tissues (such as nerves or organs) with damaged or reduced blood supply (ischemia).
Symptoms differ depending on the size and position of the damaged blood vessels and the degree of damage to the organs involved. There may be, for example, the following:
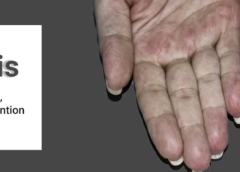
- Skin: rash with bluish-purple patches (haemorrhages) or blotches (purpura), hives, small bumps (nodules), red spots (petechiae), dilated blood vessels (livedo reticularis), or sores (ulcers) on the lower legs.
- Peripheral nerves: tingling, numbness, or weakness in the affected limb.
- Brain: Confusion, seizures, and strokes.
- Digestive tract: stomach pain, diarrhoea, nausea, vomiting, and blood.
- Heart attacks: Angina and heart attack.
- Kidneys: elevated blood pressure, fluid accumulation (edema), and defective kidneys.
- Joints: discomfort or swelling between joints.
When to Call a Professional
If you experience unexplained fever, weight loss, exhaustion, or malaise (a general feeling of sickness), with or without areas of rash, muscle weakness, breathing problems, chest pain, or other symptoms mentioned above, call your doctor.
Causes
What causes vasculitis is not entirely clear but genetics, infection and the immune system tend to play a role.
The immune system, which is the part of the body that normally battles infection, can attack cells of the blood vessel by mistake resulting in inflammation. Many medical professionals believe that vasculitis is an autoimmune disorder.
Vasculitis can affect individuals of any age, race, or gender. Smoking and living with a chronic infection, such as infectious hepatitis, can put you at an increased risk of developing vasculitis. Cancer, other drugs, and other illnesses are known to cause inflammation can also cause vasculitis.
Risk factors
Doctors do not know exactly why Vasculitis happens. Vasculitis may occur at any age, or in any sex or race. But the risk can increase by some factors, such as:
- Having autoimmune disorders like lupus, rheumatoid arthritis, and scleroderma.
- Medicines.
- Having Infections like hepatitis B, hepatitis C, or viral illness.
- Blood cancers.
- Smoking
Vasculitis complications
Vasculitis can cause damage to the blood vessels, rendering them thick, thin, narrow, or scarred. It will restrict blood flow so that the organs and tissues do not get the oxygen and nutrients they need. Many humans can never suffer vasculitis complications.
Many patients may encounter problems with arthritis, nose, or sinus. Stronger risks include:
- Vision loss or blindness.
- Infections like pneumonia and sepsis (blood infection).
- Limb loss.
- Organ damage including to lungs, heart, kidneys or brain
- Blood clots and aneurysms
Can You Prevent Vasculitis?
The following suggestions may help:
- Choose a healthy diet. Eating healthy may help avoid possible complications, such as thinning bones, high blood pressure, and diabetes, that may arise from your medications. Select a diet featuring fresh fruits and vegetables, whole grains, low-fat dairy products, and lean meats and fish. When you are taking a corticosteroid drug, ask your doctor if you need to take a supplement of vitamin D or calcium.
- Get routine vaccinations. Being up to date on vaccines such as the flu and pneumonia may help avoid complications that may result from the medications, such as infection. Chat about vaccines with your doctor.
- Exercise most days of the week. Regular aerobic activity, such as walking, can help you reduce bone loss, hypertension, and diabetes that could be associated with corticosteroid usage. This protects your heart and your lungs too. Furthermore, many people find that exercise boosts their mood and overall sense of health. If you don’t perform the exercise, continue slowly, and gradually build up. The doctor will help you prepare the correct fitness program.
- Maintain a strong support system. As you cope with this condition friends and family can help you. If you think it would be helpful to talk with other people who are living with vasculitis, ask a member of your health care team about connecting with a support group.
- Understand your condition. Know about vasculitis and its treatment all you can. Know the possible side effects of the medications you are taking, and inform your doctor about any changes in your health.
- Go ahead with your treatment plan. Your treatment plan could include daily visits to the doctor, more tests, and blood pressure checks.
Leave a Reply
You must be logged in to post a comment.